Body Dysmorphic Disorder (BDD)
Body Dysmorphic Disorder (BDD) is a serious and complex mental health disorder. It was first described in the late 1800s by Italian psychiatrist Enrico Morselli, who called it dysmorphophobia (“fear of ugliness”). Today, BDD is categorized in the DSM-5 as an Obsessive-Compulsive and Related Disorder.
BDD incorporates biological, psychological, and sociocultural factors. It is characterized by an intense preoccupation with one or more perceived flaws in appearance. The flaw is either unnoticeable to others or, if visible, is not as significant as the individual believes.
The Cycle of BDD: How Compulsions Keep It Going
Like OCD, BDD follows a cycle. It often begins with an intrusive thought such as “My skin looks hideous” or “My nose is deformed.” This brings intense anxiety or shame.
To relieve this distress, individuals engage in compulsions, which are mental or physical actions meant to reduce anxiety. Common compulsions include:
● Checking mirrors repeatedly
● Camouflaging or covering up the ‘flaw’
● Comparing themselves to others
● Asking for reassurance
● Avoiding mirrors, photos, or social situations
These compulsions ease distress only temporarily. Soon, the intrusive thoughts and anxiety return, sometimes even stronger, which keeps the cycle alive.
Impact of BDD
BDD is more common than many realize, affecting about 1 in 50 people in the U.S. Individuals often feel defined by their perceived flaw, leading to shame, anxiety, depression, and extreme self-consciousness.
● 60% of people with BDD also meet criteria for major depression. (Phillips, Menard, Fay, & Weisberg, 2005).
● About 80% report suicidal thoughts, and about 1 in 4 have attempted suicide. (Phillips et al., 2005).
● BDD often co-occurs with OCD, eating disorders, and social anxiety.
Muscle Dysmorphia: A Subtype of BDD
A specific form of BDD is Muscle Dysmorphia, sometimes called ‘reverse anorexia.’ Individuals believe their body is too small or weak, even if they are muscular.
They may:
● Exercise or weightlift excessively
● Follow rigid diets or use steroids/supplements
● Avoid situations where their body might be seen
The DSM-5 notes muscle dysmorphia is more common in men but can affect any gender. Like other forms of BDD, it can significantly impair daily life and health
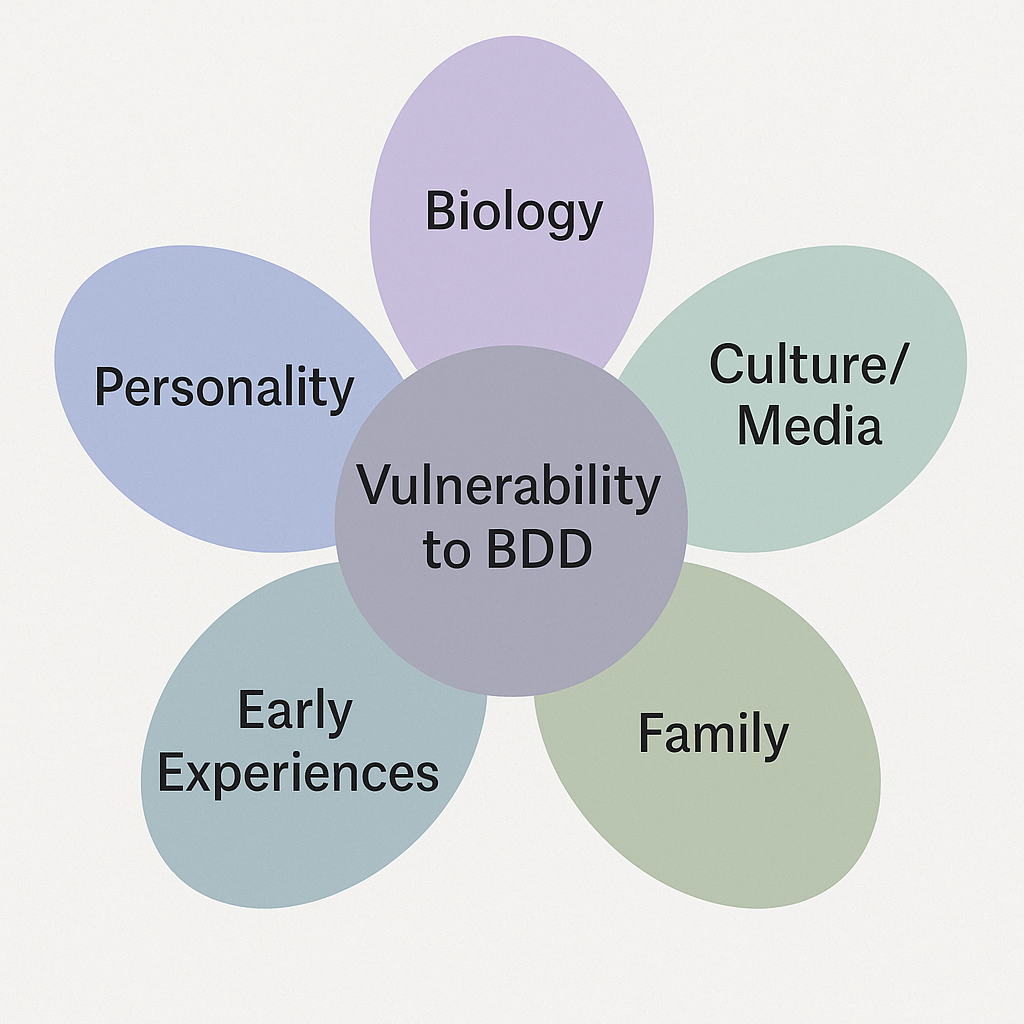
Why BDD Develops: The Flower Model
Leading researchers and therapists, David Veale, PhD and Rob Wilson, PhD, use a flower diagram to explain BDD’s development. Each petal represents a factor
● Biology, including genetics
● Personality traits (perfectionism, self-criticism, sensitivity to rejection)
● Early experiences: bullying, teasing, trauma
● Culture and media: beauty ideals, comparison culture
● Family environment: critical or appearance-focused dynamics
No single petal causes BDD. But when several overlap, the ‘flower’ of BDD grows. Therapists often use this model to help clients reflect on their own petals, which reduces self-blame.
Neuroscience of BDD
Research shows that people with BDD process visual information differently from others. Most people see their face as a whole first, then notice details. People with BDD do the opposite, zooming in on small details and missing the bigger picture. Brain scans suggest they may rely more on the left hemisphere, which is detail-focused, rather than the right hemisphere, which processes the overall picture (Phillips et al., 2010).
Other brain regions tied to fear and repetitive behaviors are also more active in BDD. This combination makes appearance concerns feel threatening and creates a powerful urge to check or fix perceived flaws (Feusner et al., 2007).
This means people with BDD are not imagining things. Their brains truly process visual input differently, which can make minor features appear magnified and overwhelming (Feusner et al., 2010).
BDD and Trauma
Many people with BDD report histories of trauma, especially in childhood. Experiences may include emotional neglect, abuse, sexual trauma, or chronic bullying. These can leave deep imprints on self-image and body perception.
● Over 75% of people with BDD report some form of abuse or neglect (Weingarden & Renshaw, 2016).
● 61% report emotional abuse, ~60% physical neglect (Weingarden & Renshaw, 2016).
● Among adolescents, about 40% report trauma exposure, compared to 18% of those with OCD (Wong & Rapee, 2016).
Trauma can amplify shame, self-criticism, and hypervigilance about perceived flaws. While it does not directly cause BDD, it is often a major contributing factor, highlighting the importance of trauma-informed care.
Treatment for BDD
BDD is highly treatable. Evidence-based treatments include:
● Psychoeducation – Learning what BDD is, how the cycle works, and why rituals keep it alive.
● Cognitive Restructuring – Identifying and challenging distorted BDD beliefs, replacing them with more balanced thoughts.
● Mindfulness – Learning to notice BDD-related thoughts without judgment and allowing them to pass.
● Exposure and Response Prevention (ERP) – Gradually facing avoided situations (e.g., going out without camouflaging) while resisting compulsions.
● Mirror Retraining (Perceptual Retraining) – Viewing oneself holistically in the mirror instead of zooming in on flaws, reducing both avoidance and compulsive checking.
● Medication – SSRIs are often prescribed; many respond best when medication is combined with therapy.
For some, progress is rapid when treatment is targeted and consistent, sometimes in 20 sessions or fewer. More complex cases, especially with co-occurring disorders, may take longer.
Final Word
BDD is not vanity; it is a painful and often misunderstood disorder that can profoundly disrupt lives. It arises from a mix of brain differences, genetics, environment, and sometimes trauma.
The good news is that BDD is treatable. With treatments such as CBT, ERP, cognitive restructuring, mindfulness, mirror retraining, and, when needed, medication, individuals can break the cycle of BDD, reduce suffering, and reclaim their lives.
References
Bjornsson, A. S., Didie, E. R., & Phillips, K. A. (2010). Body dysmorphic disorder. Dialogues in Clinical Neuroscience, 12(2), 221–232.
Wilhelm, S., Phillips, K. A., Didie, E. R., Buhlmann, U., Greenberg, J. L., Fama, J. M., & Keshaviah, A. (2012). Modular cognitive–behavioral therapy for body dysmorphic disorder: A randomized controlled trial. Behavior Therapy, 43(2), 263–277.
Wong, Q. J. J., & Rapee, R. M. (2016). The aetiology and maintenance of body dysmorphic disorder: A review of risk factors and psychological models. Clinical Psychology Review, 50, 36–46.
Weingarden, H., & Renshaw, K. D. (2016). The link between body dysmorphic disorder and childhood maltreatment: Evidence, explanatory models, and treatment implications. Clinical Psychology Review, 47, 1–10.
Feusner, J. D., Townsend, J., Bystritsky, A., & Bookheimer, S. (2007). Visual information processing of faces in body dysmorphic disorder. Archives of General Psychiatry, 64(12), 1417–1425.
Feusner, J. D., Hembacher, E., Moller, H., & Moody, T. (2010). Abnormalities of object visual processing in body dysmorphic disorder. Psychological Medicine, 40(2), 389–400.
Phillips, K. A., et al. (2010). A randomized placebo-controlled trial of fluoxetine in body dysmorphic disorder. Archives of General Psychiatry, 67(4), 317–326.
Phillips, K. A., Menard, W., Fay, C., & Weisberg, R. (2005). Demographic characteristics, phenomenology, comorbidity, and family history in 200 individuals with body dysmorphic disorder. Psychosomatic Medicine, 67(5), 670–676.
Phillips, K. A., Coles, M. E., Menard, W., Yen, S., Fay, C., & Weisberg, R. B. (2005). Suicidal ideation and suicide attempts in body dysmorphic disorder. Journal of Clinical Psychiatry, 66(6), 717–725.